Every time your pet visits the veterinarian for a procedure, you have to make a decision: what type of anesthesia will be used? While all anesthetics carry some risks, knowing the differences between them can help you make the best decision for your pet. In this blog post, we’ll take a look at the different types of anesthesia and their risks. We’ll also provide some tips on how to reduce those risks.
For some pet owners, discussions about procedures that involve anesthesia can be stressful. Many of us have heard stories about life-threatening complications that can arise due to sedation, and it makes us worry for our own pets when anesthesia is necessary for certain procedures. The use of anesthesia can be especially worrying when your pet is a little older and not as resilient.
In this article we cover the topics that every pet owner needs to know about anesthesia and the risks for their pet. What anesthesia entails, and when is it needed. The risks of administering anesthesia, and the ways that your veterinary team works to keep your dog or cat safe while under anesthesia.
What is anesthesia?
Anesthesia is the use of a combination of medications to induce sedation, tranquilization, or a state of unconsciousness for certain medical or surgical procedures. There are three types of anesthesia: local, regional, and general anesthesia.

Local Anesthesia
Local anesthesia is when one small part of the body is numbed. This type of anesthesia can be utilized when a small bump or skin tag needs to be removed. It involves the injection of a numbing agent like lidocaine. Some pets can be completely awake for this while others may need mild sedation if they are anxious or scared.
Regional anesthesia
Regional anesthesia is utilized more in human medicine than veterinary medicine. It is used to block pain in a certain area of the body. In humans, epidurals are an example. Dogs can benefit from regional anesthesia in certain kinds of painful surgeries like knee or back surgery.
General anesthesia
Patients are completely unconscious for procedures performed under general anesthesia. A short-acting induction agent is given and then the unconsciousness is maintained with inhaled gas anesthesia like sevoflurane. Invasive surgical procedures, orthopedic procedures, and dental prophylaxes are all examples of procedures that should be performed under general anesthesia. In orthopedic procedures, it is common to combine regional anesthesia with general anesthesia.
When is it necessary to use anesthesia for a pet?
For veterinarians in general practice, there are several types of procedures that can be performed such as spays/neuters, mass removals, bladder stone removals, dental prophylaxes, other soft tissue surgeries like spleen removal, and sometimes orthopedic procedures like knee surgery.
All of these require the use of general anesthesia because the patient needs to be completely still. Anesthesia also helps to mitigate pain and discomfort.
Deep dental cleaning often needs general anesthesia too. Many pet owners ask about dental cleanings for their pet while he or she is conscious. These types of cleanings are not true dental prophylaxes because deep cleaning below the gumline is necessary in order to be effective. If a cleaning is performed while the pet is awake, the cleaning will not be effective at all, nor will it provide an opportunity to look for endodontic disease with the use of dental x-rays.
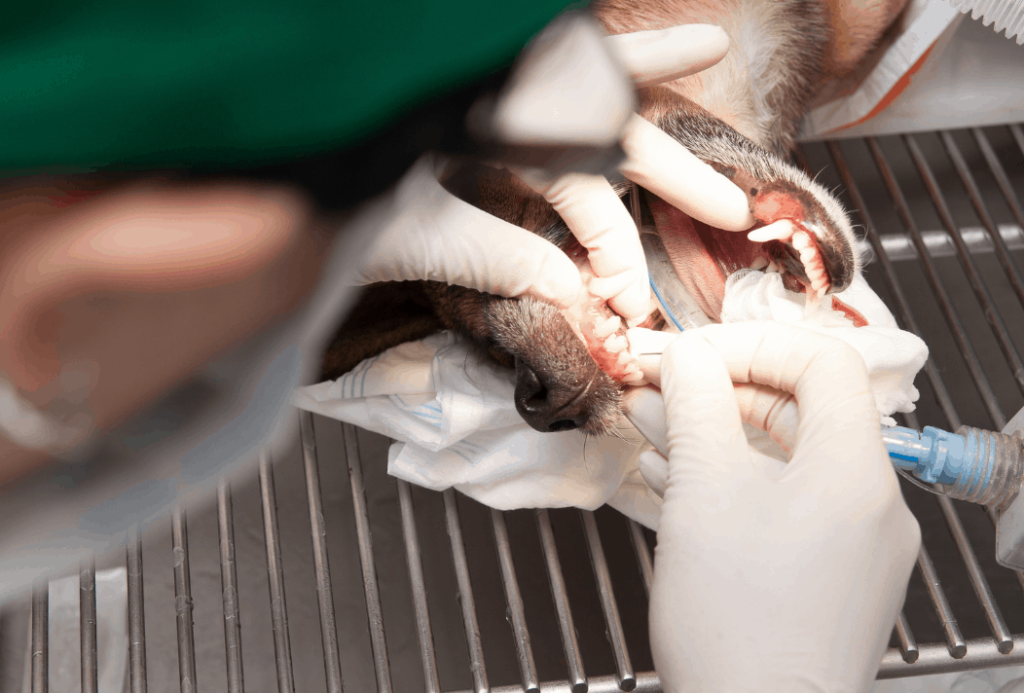
Anesthesia risks and precautionary measures
Every cat and dog is different and will have varied risk factors. This means that an older pet or a pet with heart disease, kidney disease, etc. should not receive the same anesthetic protocol as a very young, healthy pet. Your veterinarian will evaluate your cat or dog and determine which protocol is best. For more information about some of the common diseases that interfere with anesthesia, we recommend the articles on liver disease in dogs, liver disease in cats, kidney disease in cats, kidney disease in dogs, or heart disease in dogs.
ASA Scoring System
Most veterinarians use the ASA scoring system to determine a pet’s anesthetic risk and how best to proceed. The ASA system was adapted from human medicine from the American Society of Anesthesiologists and scores a patient from one to five, with five being the highest risk for complications due to general anesthesia.
- Class 1 – young and/or healthy patient (minimal risk)
- Class 2 – mild systemic disease; usually seniors, neonates, or obese patients (slight risk)
- Class 3 – moderate systemic disease; low-grade heart murmur, anemia, fever (moderate risk)
- Class 4 – severe systemic disease; severe heart disease, shock, lung disease, uncontrolled diabetes, end-stage kidney disease (high risk)
- Class 5 – extreme risk of complications but patient might die without surgery
- Class E – emergency status, can be attached to the other classes (e.g. ASA 2E)
Pre-anesthetic blood work
Pre-anesthetic blood work can help rule out underlying illness before it becomes a problem. It can look for white blood cell count, red blood cell count, platelet count, liver enzymes, kidney values, proteins, blood sugar, etc. If blood parameters are abnormal, your vet may recommend additional testing or take special precautions to minimize the risk of anesthetic complications.
Caution when administering sedative medications
Some of the medications that are used as sedatives prior to induction can cause decreases in heart rate and blood pressure. Medications like acepromazine should not be used in patients with heart disease, liver disease, or kidney disease, and it should be used with caution in brachycephalic breeds. Induction agents like propofol should be administered slowly; otherwise, it may cause apnea which is when breathing stops completely.
Monitoring vitals
Monitoring a patient’s vitals during anesthesia is extremely important. Many veterinary staff are trained to monitor heart rate, respiratory rate, blood pressure, and oxygen saturation. An electrocardiogram or EKG can be continuously monitored to look for heart arrhythmias, and temperature is monitored to ensure that a patient doesn’t become too cold. Intravenous fluid support can minimize the risk of low blood pressure or hypotension, especially due to blood loss.
Recovery and post-surgery is a critical time
The most likely time for complications to arise is during recovery or post-surgery, especially in cats. Temperature, heart rate, and respiratory rate should be closely monitored while the patient recovers. If severe blood loss occurred, a blood transfusion may be necessary. If a patient is in extreme pain, additional pain medications can be given. Hypothermic patients can be kept warm with towels or heating apparatuses.

Many patients are expected to stay in the hospital for at least five to six hours before going home. More severe surgical procedures may require that your pet remain hospitalized for a day or two post-surgery. The goal for same-day procedures is that patients should be able to walk without assistance. Some may be tired or groggy for a day or two while others go right back to having normal energy that evening!
Making an informed decision on the risk of anesthesia for your cat or dog
Anesthetic protocols are not intended to be “one size fits all.” Your veterinarian will help you weigh the pros and cons of general anesthesia and will discuss the risks with you.
Thanks to the many technological advances in veterinary medicine and anesthesiology, the risk of anesthetic complications and anesthetic death are much lower. If you have concerns or other questions, contact your veterinarian to express your concerns and figure out what approach will be best for your furry family member.









